Life-Saving Incentives: Consequences, Costs and Solutions to the Organ Shortage
By Alexander Tabarrok

Consequences and costs
“Our current organ procurement system is a terrible failure. Organs that could dramatically extend lives and return the sick to health are routinely wasted.”
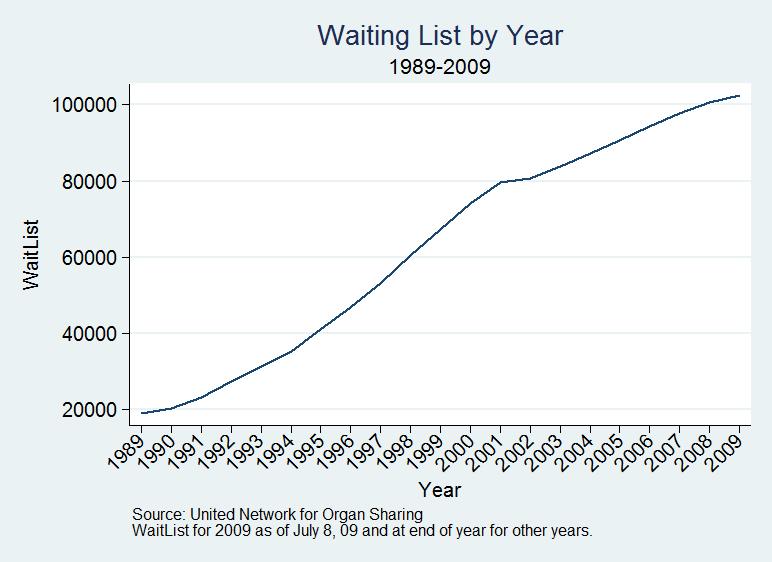
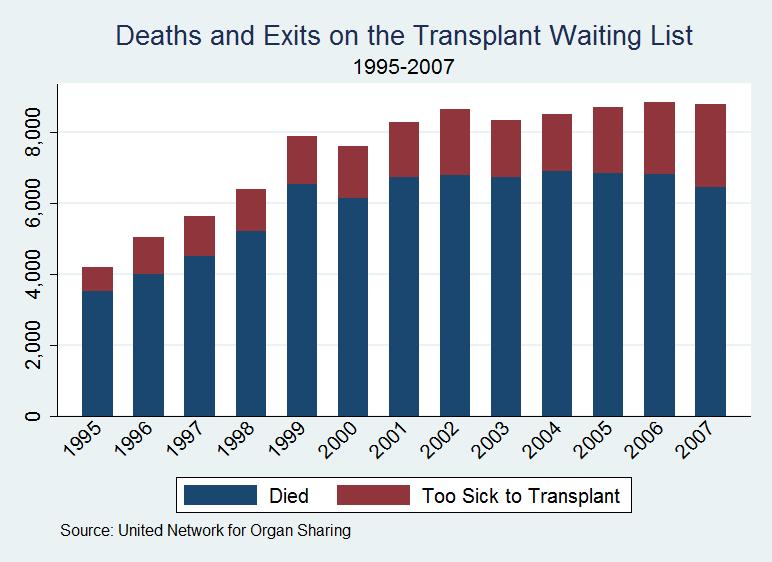
Even this higher figure is an underestimate of the deaths due to the shortage because many people who could benefit from an organ transplant are never put on the waiting list in the first place because their physicians know that the probability of obtaining an organ is low.1 The shortage of organs has other costs in addition to the deaths of those waiting for a transplant. Most obviously, the shortage greatly reduces the quality of life for those on dialysis or otherwise waiting for a transplant.
The shortage of organs has also increased the use of so-called “expanded-criteria” organs, organs that used to be considered unsuitable for transplant. Kidneys donated from people over the age of 60 or from people who had various medical problems are more likely to fail than organs from younger, healthier donors but are now being used under the pressure of the shortage. Expanded-criteria organs are a useful response to the shortage; but their use also means that the true shortage is even worse than it appears because as the waiting list lengthens, the quality of transplants is falling.
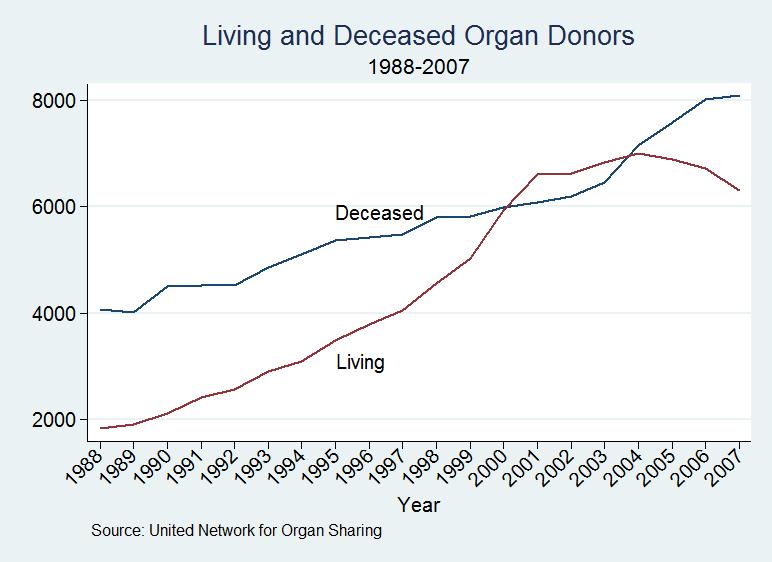
Another, rarely-acknowledged cost of the shortage is the increased use of living donors. In 2001, for the first time ever, the number of living donors exceeded the number of cadaveric donors although the number of living donors has since declined (see Figure 3).2 I greatly admire and respect all who choose to donate an organ (primarily kidneys although parts of a liver can also be donated). But it is a travesty that living bodies are medically harmed while at the same time perfectly acceptable cadaveric organs are wasted. All else being equal, reliance upon cadaveric organs is preferable to risking the health of living donors.3 If more cadaveric donations were made available, the necessity of living donations would fall.
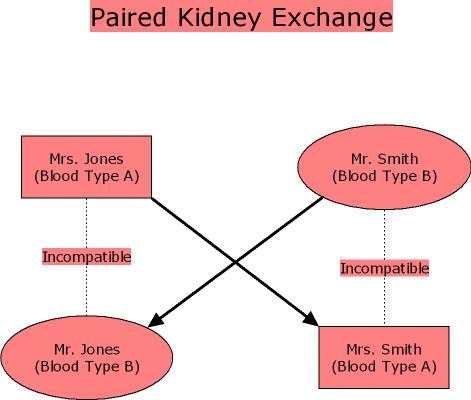
The greater demand for living donors has generated an important innovation, kidney swaps. Imagine that your spouse is dying of kidney disease. You want to give her one of your kidneys but tests show that your kidney is incompatible with her immune system. Utter anguish and frustration. Is there anything that you can do? Today the answer is yes. Transplant centers are now helping to arrange kidney swaps. You give to the spouse of another donor who gives to your spouse. Figure 4 illustrates. Even a few three-way swaps have been conducted.4 Overall, however, only about 150 such swaps have been performed in the United States since 2000.5 More efficiency in kidney allocation is desirable but greater efficiency alone will not lift the shortage of organs.
A longer waiting list for an organ transplant is not necessarily a bad thing; in two respects it is a sign of success. On the demand side, better surgical techniques and improved anti-rejection drugs have meant that many more people could benefit from an organ transplant if one were available. The demand for organs grows as medical knowledge advances. On the supply side, improved auto safety and a falling homicide rate have reduced the base supply of cadaveric organs (Perez-Pena 2003). No one wants to reduce medical progress or increase the number of auto accidents, so longer waiting lists are not entirely to be bemoaned.
Nevertheless, our current organ procurement system is a terrible failure. Organs that could dramatically extend lives and return the sick to health are routinely wasted. In the United States, less than one half of potential organ donors became actual organ donors (Sheehy et al. 2003, Evans et al. 1992). The shortage of organs could be greatly alleviated, and eliminated entirely for at least some organs, if more people were to sign their organ donor cards and if more families agreed to donate after the death of a loved one.
Causes and Solutions to the Shortage
Repeated exhortations from the government and organizations interested in organ procurement, including campaigns featuring Michael Jordan as a spokesperson, have not greatly increased organ donation in the past and are unlikely to do so in the future. Solving the organ shortage will require more innovative thinking and a willingness to question convention.
Better Incentives
Our current organ procurement system relies solely on altruism to motivate donation. Altruism is a fine thing but it is in short supply. We may hope for love but should plan on self-interest.
Incentives for organ donation can take a variety of forms. Financial compensation is the most discussed option but reciprocity proposals are another possibility that I discuss further below. It is currently illegal to compensate donors or their families for organ donation. To be precise, the National Organ Transplant Act (NOTA) of 1984 states “It shall be unlawful for any person to knowingly acquire, receive, or otherwise transfer any human organ for valuable consideration for use in human transplantation.”6
But due to the increasing shortage, support for changing NOTA is growing. The American Medical Association, The American Society of Transplant Surgeons and The United Network for Organ Sharing (UNOS), among other groups have all come out in favor of at least testing the idea of financial compensation. Congress has recently debated several bills to this effect albeit without passage. Nevertheless, I predict that as the shortage of human organs grows so will support for allowing financial compensation.
Types of Financial Incentives
In the minds of many, financial incentives for organ donation mean rich people buying up kidney’s that are being hawked on eBay by the desperately poor. In reality, we need make only marginal changes to the current system in order to create a revolution that would save many lives. Two distinctions are especially important. First, financial compensation for cadaveric donation and for living donation are different ideas and it is quite possible to have one without the other. Indeed, the primary cause of so-called organ tourism—rich people flying to poor countries like India to undergo a transplant from a poor, living donor—is the shortage of organs in the West. By allowing compensation for cadaveric donations we’ll increase the domestic supply and reduce the demand for people to fly to poorer countries for living. Financial compensation for cadaveric donation, in other words, is a substitute for both paid and unpaid living donation.7
Second, it’s possible to pay organ donors, whether living or deceased, without allocating organs based on financial payment. Transplant organs, for example, are currently allocated according to a point system which is based on factors such as the quality of the match between donor and recipient, the length of time the potential recipient has been on the waiting list, the health of the potential recipient, the location of the recipient and donor and so forth. It is not necessary to change these criteria in order to make use of financial compensation. Donors can be compensated, for example out of government funds, and the organs can still be allocated according to a point system.
Financial incentives can be divided into forward-looking approaches and on-the-spot approaches.
Forward-looking approaches
Forward approaches involve offering some type of incentive for people to become part of an organ donor registry so that if they die under circumstances where they can donate, their organs will be recovered. An incentive to donate, for example, could be created by something as simple as offering a discount on driver’s licenses to those who sign up to be an organ donor. At one time Georgia offered a paltry discount of $9 on the license fee but that program has since been discontinued in order to increase state revenues.
An options market in organs would allow firms to buy the rights to organs in the event of the donor’s death (Cohen 1995, Barnett, Blair, Kaserman 1996). Every potential donor would either be paid a small amount today to join the registry or would register today in return for the possibility of much larger payments to his estate should he become an actual donor. An options market, therefore, would work much like life insurance (which used to be called “death insurance,” a more accurate if less appealing name). The advantage of an options market, over an arbitrarily-chosen license fee discount or similar plan, is that firms would have an incentive to promote donation and the prices offered would automatically increase as shortages become more severe. Payments for the organs would ultimately be made by insurance companies and government just as for other medical services. (See further below on the costs of financial compensation plans.)
An advantage that all forward-looking approaches share is that the autonomy of the donor is maximized and the decision-making burden is taken off family members at that most difficult time, when they have just learned that their loved one is brain-dead. And, fortunately, experience shows that when families are informed of their loved one’s wishes, they almost always assent to the donation (Siminoff et al. 2001).
On-the-Spot approaches
“On-the-Spot” incentives are offered only to the families of people who are suitable deceased donor candidates. The American Society of Transplant Surgeons, for example, has said that it would be ethically acceptable to offer to make a charitable contribution on behalf of the deceased or to cover the funereal expenses of deceased organ donors (Arnold et al. 2002). In my judgment, a direct payment to the estate of the deceased would also be ethically acceptable. Payments of this kind can be given as a way of saying thanks for the sacrifice the family has made in service to the community and would be similar to the death benefit offered to the families of people in the military who die in the line of duty.
For example, the Ad Hoc Committee to End the Intractable Shortage of Human Organs, of which I am a member, has recommended a gift for the gift of life that would go the estate of deceased organ donors. We have suggested that the following type of language should be used in approaching the family of a potential donor.
Dear Mr. Smith/Ms. Jones, as you may know, it is our standard policy to offer a gift of $5,000 to the estate of the deceased, as a way of saying “Thank you for giving the gift of life.” The money can be used to help offset funeral or hospital expenses, to donate to your loved one’s favorite charity, or simply to remain with the estate, to be used in any manner the heirs see fit. No price can be placed upon the many lives that can be saved by your gift. Our donation in return is merely society’s way of honoring the sacrifice you are being asked to make, and is a token of our deep and sincere appreciation for your generosity at this most difficult time.
Evidence on Incentives in Organ Donations
A little-noted peculiarity of our current system is that some forms of compensation for whole body donation are legal even though compensation for organs is not. In many states, for example, medical schools offer free cremation services to families that donate bodies for medical research. Thus we have the bizarre situation where a medical school can compensate a donor for their whole body, if they use the body for teaching, but if they use an organ from that same body to save a life that would be illegal.8
Whole body donation also lets us test the hypothesis that incentives will increase donation rates. Funeral services are more expensive in some states than in other states so the offer to cremate a body after whole body donation is more valuable in some states than in others. Consistent with the hypothesis that incentives work, whole body donation is more common in states with more expensive funerals (Harrington and Sayre 2006-2007).
Incentives also appear to work for living organ donation. Only one country in the world has legalized financial payments to kidney donors. And only one country in the world has eliminated the shortage of transplant kidneys Surprisingly, that country is Iran.
In the Iranian system organs are not bought and sold at the bazaar. Instead a non-profit, volunteer-run Dialysis and Transplant Patients Association (DATPA) mediates between recipients and donors. Recipients who cannot be assigned a kidney from a deceased donor and who cannot find a related living donor may apply to the DATPA. The DATPA identifies a possible donor from a pool of people who have applied to the DATPA to be donors. Donors are medically evaluated by transplant physicians, who have no connection to the DATPA, in just the same way as are non-financially compensated donors.
The government pays donors $1,200 plus limited health insurance coverage. In addition, charitable organizations also provide remuneration to impoverished donors and recipients may also contribute to donor remuneration. The system appears to work well, as noted above, Iran is the only country in the world without a shortage of human organs.9
Saving money while saving lives
In this age of expensive medical care, many people wonder whether financial compensation for organ donation would be too expensive. In fact, we can save money while saving lives. Kidney transplants are cheaper than dialysis over prospective lifetimes and they pay for themselves within 2-3 years (Schweitzer et al. 1998, Loubeau et al. 2001, Matas and Schnitzler 2004). Most of the costs of dialysis are paid for by the Federal government through the End Stage Renal Disease (ESRD) program. Thus, any increase in organ supply automatically reduces costs to the Federal government. Becker and Elias (2007) estimate that at a price of $15,000 paid to live donors the shortage of kidneys could be ended entirely. Payments to deceased donors or their estates would presumably increase the supply at a much lower price. But each additional kidney saves the Federal government approximately $100,000 so organ payments would save millions of dollars per year.10 Thus on a pure financial basis paying donors pays for itself. More importantly, increases in organ donation would allow more dialysis patients to live longer, better lives. Adding in the value of these additional quality-years would significantly increase the value of donation.
Reciprocity Plans
The economics of common resources provides another perspective on the shortage of organs. Resources owned in common tend to be under-supplied and over-utilized. No one wants to pay to restock a lake, for example, when the benefits of restocking flow to everyone regardless of whether or not they helped to pay for the restocking. As a result, open fisheries are almost always driven to depletion. The solution is to close the fishery to those who do not help to restock the lake.
UNOS considers organs to be a “national resource,” owned in common. The result, as in other areas, is a tragedy of the commons. Everyone wants to fish in the organ pool but no one has a direct incentive to “restock the lake” by signing their organ donor card. As with fishing lakes, a solution to this problem is to close the organ pool to non-donors.
Consider a no-give, no-take policy for organs (Tabarrok 2002, Gubernatis and Kliemt 2000). Under this system in order to receive an organ you must have previously signed your organ donor card.11 Under no-give, no-take, signing your organ donor card can be thought of as joining a club, the club of people who have agreed to share their organs. Or one can think of signing the organ donor card as the price that you pay for organ insurance.
An advantage of the no-give, no take policy is that it satisfies most people’s moral intuitions. Many people find the idea of paying for organs distasteful but nevertheless are comfortable with the morality of reciprocity, those who are willing to give should be the first to receive.
A variant of no-give, no-take can be implemented quite easily within the current system by giving those who have previously signed their organ donor cards extra points that would advance them on the queue. In fact, a similar program is already in place. People who have previously been live organ-donors are given extra-points should their one remaining kidney fail them. No-give, no-take simply extends this idea from actual donors to potential donors.
Something like no-give, no-take is currently being implemented privately. Lifesharers.com is an “organ club.” Anyone can join.12 Members agree that if their organs should become available they will go first to a fellow Lifesharers member. (If everyone joins Lifesharers, it becomes equivalent to no-give, no-take.)
Although reciprocity proposals like no-give, no-take have moral advantages it is important to remember that their primary purpose is to increase the incentive to donate and therefore to increase the total number of organs available.
Conclusion
For a podcast on organ donations, see The Economics of Organ Donations with Richard Epstein. EconTalk, June 5, 2006.
An earlier version of this article was published in 2004 and is available at Life-Saving Incentives: Consequences, Costs and Solutions to the Organ Shortage.
Adam Smith noted that in his time there were “some very agreeable and beautiful talents of which the possession commands a certain sort of admiration; but of which the exercise for the sake of gain is considered, whether from reason or prejudice, as a sort of public prostitution.” As examples, Smith lists acting, opera singing and dancing. Today the list strikes us as peculiar, perhaps even foolish. What could possibly make opera singing admirable when done for free but despicable when done for pay?
And yet, however peculiar the views of Adam Smith’s contemporaries were on financial compensation for opera singers we can at least say this in their favor—no one ever died because of a shortage of singers.
Arnold, R. et al. 2002. Financial Incentives for Cadaver Organ Donation: An Ethical Reappraisal. Transplantation 73 (8):1361-67.
Basinger, B. 2003. Organ Donor Discount Could End. Savannah Morning News Feb. 06, 2003. Available at: SavannahNow.com.
Becker, G. and J.J. Elías. 2007. Introducing Incentives in the Market for Live and Cadaveric Organ Donations. Journal of Economic Perspectives 21 (3): 3-24.
Cohen, Lloyd R. 1995. Increasing the Supply of Transplant Organs: The Virtues of an Options Market. New York: Springer; Austin: R. F. Landes.
Barnett, A. H., R. D. Blair, and D. L. Kaserman. 1996. A Market for Organs. Society 33 (6):8-17. Reprinted In Entrepreneurial Economics: Bright Ideas from the Dismal Science, ed. A. Tabarrok. 2002. Oxford: Oxford University Press.
Evans, R. W., C. E. Orians, and N. L. Ascher. 1992. The Potential Supply of Organ Donors: An Assessment of the Efficacy of Organ Procurement Efforts in the United States. Journal of the American Medical Association 267 (2):239-46.
Epstein, R. A. 1993. Organ Transplants: Is Relying On Altruism Costing Lives? The American Enterprise 50 (October/November):51-57.
Gubernatis, G., and H. Kliemt. 2000. A Superior Approach to Organ Allocation and Donation. Transplantation 70 (4):699-707.
Harrington, David E. and E. A. Sayre. 2006-2007. Paying for Bodies, But Not for Organs. Regulation 29 (4); 14-19. PDF file.
Hippen, Benjamin. 2008. Organ Sales and Moral Travails: Lessons from the Living Kidney Vendor Program in Iran. Cato Policy Analysis no. 614. Available online at http://www.cato.org/pub_display.php?pub_id=9273.
Loubeau, P. R., J. M. Loubeau, and R. Jantzen. 2001. The Economics of Kidney Transplantation Versus Hemodialysis. Prog Transplant 11 (Dec):291-97.
Matas, A. J., and M. Schnitzler. 2004. Payment for Living Donor (Vendor) Kidneys: A Cost-Effectiveness Analysis. American Journal of Transplantation 4 (2):216-21.
Perez-Pena, R. 2003. Downside to Fewer Violent Deaths: Transplant Organ Shortage Grows. The New York Times 2003 (19 August):B1.
Roth, A.E. T. Sönmez and M. U. Ünver. 2004. Kidney Exchange. Quarterly Journal of Economics, 119: 457-488.
Roth, A.E., T. Sönmez and M. U. Ünver. 2005. A Kidney Exchange Clearinghouse in New England. American Economic Review 95 (2): 376-380.
Schweitzer, E. J. et al. 1998. The Shrinking Renal Replacement Therapy “Break-Even” Point. Transplantation 66 (8):s5.
Sheehy, E., S. L. Conrad, L. E. Brigham, R. Luskin, P. Weber, M. Eakin, L. Schkade, and L. Hunsicker. 2003. Estimating the Number of Potential Organ Donors in the United States. New England Journal of Medicine 349 (7):667-74.
Simnoff, L. A., N. Gordon, J. Hewlett, and R. M. Arnold. 2001. Factors Influencing Families’ Consent for Donation of Solid Organs for Transplantation. Journal of the American Medical Association 286:71-77.
Tabarrok, A. 2002. The Organ Shortage: A Tragedy of the Commons. In Entrepreneurial Economics: Bright Ideas from the Dismal Science, ed. A. Tabarrok. Oxford: Oxford University Press.
URREA; UNOS. 2002 Annual Report of the U.S. Organ Procurement and Transplantation Network and the Scientific Registry of Transplant Recipients: Transplant Data 1992-2001 [Internet]. Rockville (MD): HHS/HRSA/SPB/DOT; 2003.
Data on waiting lists and related data can be found at Unos.org. There are approximately 315,000 patients participating in the End Stage Renal Disease program but only about a quarter of these are on the kidney waiting list even though in a world without shortages many more would be transplant candidates.
Although the number of living donors exceeded the number of deceased donors the living donors provide only one kidney while the deceased donors may provide two kidney as well as other organs, thus the number of transplants from deceased donors still exceeds the number of transplants from living donors.
Raw figures indicate that life expectancy at 5 years for the recipient of a living donation is higher than that for a cadaveric donation by about 10 percentage points (approx. 90 versus 80 percent). The raw figures, however, do not control for other differences between recipients of living donation and recipients of cadaveric donation. Recipients of living donation tend to be younger (think parents donating to children), spend less time on the waiting list, be better educated, and richer than recipients of deceased donation (see chapter 6 of URREA (2002)) and all of these factors would tend to raise 5 year life expectancy in this group regardless of the type of donation received. Nor do raw results control for the characteristics of the donor other than whether they are living or deceased.
But why stop at three? What about an n-way swap? Let’s add in the possibility of an exchange that raises your spouse on the queue for a cadaveric kidney. And let us also recognize that even if your kidney is compatible with your spouse’s there may be a better match. Is there an allocation system that makes all donors and spouses better off (or at least no worse off) and that maximizes the number of beneficial swaps? In an important technical paper Alvin Roth et al. (2004, 2005) describe an allocation mechanism put into place by the New England Program for Kidney Exchange that maximizes the number of beneficial exchanges.
New England Program for Kidney Exchange. NEPKE NEWS. January 2007.
National Organ Transplant Act of 1984, 42 USC 274e S. 301.
To be clear, there may be good reasons for allowing paid compensation to living donors as well as for changing the current criteria for allocating organs (see, for example, Cohen (1995), Epstein (1993). I am not arguing against either proposal only pointing out that these proposals are distinct from financial incentives for cadaveric donation.
The legality of compensation for whole body donation but not for organ donation also means that families who donate organs may be bearing a cost. Medical schools rarely accept bodies from which some organs have been harvested so organ donation means that families must sometimes pay for cremation expenses that would have been paid for by medical schools had the whole body been donated.
On Iran’s system see Hippen (2008) and references therein.
Matas and Schnitzler (2004) calculate that a living donor saves the US medical system $94,579 in present value. I have assumed that the savings from cadaveric donation would be similar; although life expectancy might be somewhat less for cadaveric donation (see note 3), the costs of donation to the donor are also lower.
Children could be considered automatic recipients until say their 18th birthday. A one-year waiting period could prevent people from waiting to sign their organ donor card until they became sick.
I am an advisor to Lifesharers.com.
*Alexander Tabarrok is the Bartley J. Madden Chair in Economics at the Mercatus Center, George Mason University, and Director of Research, The Independent Institute. He writes regularly at www.MarginalRevolution.com.